Fibromyalgia
This webpage is about functional medicine treatments for fibromyalgia. It is not about the routine medical approach. There is a brief introduction, though, providing the standard information in case you know very little about your condition.
If your fibromyalgia and fatigue treatment is working really well for you and you’re feeling wonderful then there is no need to read any further.
If your treatment is not working well for you then I think you may find the information on this page very useful – many of my patients have found this to be the case.
If you have any long-term illness
Learn as much as you can about it and become an active agent in your own healing so that, having listened to the advice of your doctor, you can make informed, wise decisions.
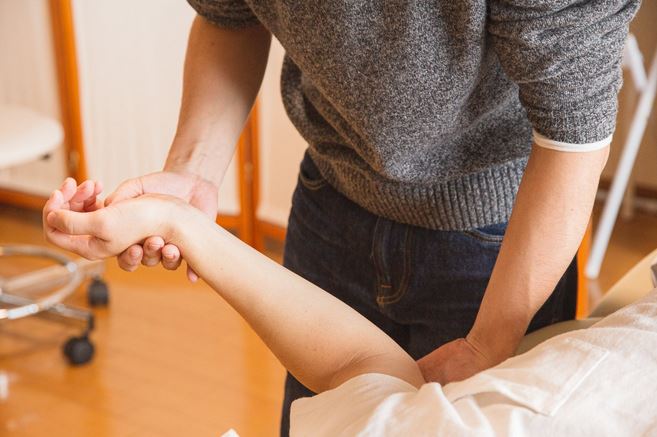
Part One: Standard medical treatment for fibromyalgia
Fibromyalgia is just really a‘label’-not useful for much more than certifying illness for occupational reasons:
- To diagnose fibromyalgia it’s important that conditions which may have seemingly similar symptoms have been ruled out. This means that conditions such as rheumatoid arthritis, osteoarthritis, Sjogrens Syndrome, systemic lupus erythematous, depression disorder, anxiety, chronic fatigue syndrome et cetera all have been ruled out.
- Especially important to rule out would be thyroid disease and chronic fatigue syndrome.
- In my opinion the real usefulness of a fibromyalgia diagnosis is that a person can be certified for medical absence/sickness benefit. The diagnosis really tells pretty well nothing about what process is going on biochemically with the person.
Standard Information on Fibromyalga
- Age and gender Fibromyalgia syndrome affects women seven times as much as it affects men
- Peak age of onsetis 35 to 45 years old.
Symptoms of fibromyalgia (Source NHS website https://www.nhs.uk/conditions/fibromyalgia/)

As well as widespread pain, people with fibromyalgia may also have: Increased sensitivity to pain, extreme tiredness (fatigue). muscle stiffness, difficulty sleeping, problems with mental processes (known as “fibro-fog” problems with memory and concentration), headaches, irritable bowel syndrome (IBS, a digestive condition that causes stomach pain and bloating)
Diagnosis of Fibromyalgia https://www.mayoclinic.org/diseases-conditions/fibromyalgia/diagnosis-treatment/drc-20354785:
The Mayo Clinic website states:
“In the past, doctors would check 18 specific points on a person’s body to see how many of them were painful when pressed firmly. Newer guidelines don’t require a tender point exam. Instead, a fibromyalgia diagnosis can be made if a person has had widespread pain for more than three months — with no underlying medical condition that could cause the pain.”
Diagnostic tests – from the Mayo Clinic Website
While there is no lab test to confirm a diagnosis of fibromyalgia, your doctor may want to rule out other conditions that may have similar symptoms.
Treatment options
- “In general, treatments for fibromyalgia include both medication and self-care. The emphasis is on minimizing symptoms and improving general health. No one treatment works for all symptoms”.
- The medications mentioned include both over-the-counter and prescription pain relievers, antidepressants and antiseizure medications.
- Other therapies which are mentioned on the Mayo Clinic site include physiotherapy, occupational therapy and counselling.
- ‘Lifestyle’ modifications also receive a mention
Outlook/prognosis ( Source NHS website https://www.nhs.uk/conditions/fibromyalgia/)
- The NHS site states somewhat ‘delicately’ : Although there’s currently no cure for fibromyalgia, there are treatments to help relieve some of the symptoms and make the condition easier to live with.
Part Two: Oriented towards patients who are not getting better and contains a detailed analysis of fibromyalgia from a functional medicine viewpoint
POSSIBLE TRIGGERS FOR FIBROMYALGIA
HORMONAL FACTORS
Hint: Don’t forget the statement above that seven women suffer from fibromyalgia for everyone male sufferer. So hormones might just be very important
- Thyroid hormone: I suggest checking free T3 , free T4 and TSH. In my opinion I don’t think the expense of looking at reverse T3 is justified because there was so little one can do therapeutically to reduce, reverse T3 levels. I prefer to put my effort into areas where it is more likely to pay off rather than getting obsessed with reverse T3.
- The Adrenals Both low and high cortisol levels may be present in fibromyalgia patients. It also is important to check DHEA levels.
- The Ovaries Many women who suffer from fibromyalgia are in the peri-, pre- or menopausal phases of life. I consider it is very important to check oestrogen and progesterone level usually both at days 2 to 5 and also at days 18 to 21 if there are any concerns about hormone levels.
INFECTIONS
- Lyme Disease and coinfections may be a trigger for fibromyalgia
- Non-specific viral illnesses and infections sometimes a patient will say:” I was just fine until I got that infection- that really set my health in a downward spiral”. Sometimes a gastrointestinal infection can be the trigger, sometimes a respiratory infection may just be the straw which breaks the camel’s back.
- Persistent/recurrent infection if this is present in a patient with fibromyalgia then I will advise: one must be suspicious of this and investigate further.
- Vitamin and mineral deficiency issues
- Low magnesium and low vitamin D may play a role in fibromyalgia in some circumstances.
- Other vitamins and minerals may also be deficient and be part of the jigsaw puzzle. An important part of finding the solution is why is this patient not absorbing their minerals/ vitamins
FOODS
- Food Intolerance may be a significant player at times and I have moved away from elimination diets to blood tests because I think a lot of patients find elimination diets emotionally very difficult. They are the gold standard of food intolerance testing but people often find them extremely frustrating.
- Fungal Toxins / Mycotoxins
- Fungal toxins/mycotoxins and fibromyalgia. There has been a lot of research done recently regarding fungal/mycotoxins and persistent inflammation. Only in the past few years have we been able to use sophisticated urinary screening to check noninvasively for fungal toxins. I have found it a huge and worthwhile advance in patient care.
TOXIC ENVIRONMENTAL CHEMICALS
- Checking environmental chemical load and glyphosate levels in the urine has been a big advance in patient treatment.
- Urinary Organic Acids Testing
- I currently use urinary organic acid testing as a screen which gives a brief look at a lot of biochemical markers- everything from evidence of abnormal gut bacteria to overworked detoxification systems
METHYLATION CHEMISTRY
- The activity of methylation which literally consists in the addition of one carbon and three hydrogen atoms, has many very diverse roles in the body and can affect functions ranging from detoxification in the liver to serotonin availability and lots more besides. Methylation alters DNA expression without having to alter the DNA itself .
HEAVY METALS
- Lead and Mercury are two heavy metals which can cause trouble in the body . There is also a suspicion that the body actually uses fungus as a defence against mercury.
- Hence it is very important if one is using antifungals to also think about ‘mopping up ‘ andeliminating from the body or any heavy metals which may become free in the process of treating the fungal overgrowth. If this is not done then the fungus may return very quickly.
TREATING FIBROMYALGIA
- Work out what is going on This is where a detailed medical history is really useful. Look at when the fibromyalgia came: What were the circumstances? Was there an infection present at the time ? Was it a time of emotional stress ? Did it coincide with some kind of dental infection ? Did it coincide with some kind of toxic exposure ? I could go on but you get the idea!
- Think Jigsaw Puzzles not Magic Bullets: Think of the patient’s problem as solving a jigsaw puzzle rather than shooting a magic bullet at the patient’s problem – consider that a combination of issues rather than one single issue is most likely causing the problem.
SOME FAIRLY TYPICAL PATIENT SCENARIOS:
*******Fibromyalgia Case History Number One*******
Let’s imagine that patient is a 48-year-old female who is going through a somewhat early menopause and she has been having menopausal symptoms for the past two years and the fibromyalgia and associated symptoms only presented about one year ago.
This lady felt very well all her life up until now. In a case like this it might be worthwhile to probably limit initial investigation and intervention to normalising vitamin and mineral status as much as possible and of course replacing the missing hormones. This alone coupled with a few nutritional medicine ‘tweaks’ might give a very nice result.
*******Fibromyalgia Case History Number Two*******
A very different case -much more complicated. Let’s suppose that this patient is male aged 40, has digestive disturbance, severe aches and pains everywhere, wakes every morning feeling tired with a low, low mood and a ‘thick’ head and this has gone on for 15 years i.e. his health has always been somewhat fragile. This person had lived in a damp house for three years in his 20s at which time the symptoms began.
This patient also has prostate symptoms, persistent sinus issues as well as the fibromyalgia symptoms. There is also chemical sensitivity and he finds that he can have a few glasses of spirits without feeling unduly sick/hungover but even small amounts of wine or beer make him feel nauseated, sick and hungover the next day.
This gentleman also finds this that his nose is “running like a tap”, sinuses are congested all the time and are uncomfortable 24/ 7 and he is suffering from frequent and severe sinus infections each winter. He feels much sicker in damp weather. There are reactions in some foods.
On the basis of medical history this person may well have a fungal issue, may well also have an environmental chemical overload, his liver maybe sluggish in terms of detoxification pathways and his toxin elimination is probably slow. Let’s say the tests come back and show fungal toxins in large amounts and also a chemical overload. Food testing shows a reaction to candida albicans.
[Other symptoms in a patient’s history which might make me suspicious of a fungal problem would include sensitivity to bright light, sensitivity to electrical shops, a metallic taste in the mouth, coughing, chest pain, shortness of breath, abdominal pain and nausea and diarrhoea. The list goes on and on!]This patient is going to need antifungals, is going to need to make sure that his home environment is clean and dry ( fungus thrives in the west and the damp) , is going to need agents to help with liver detoxification. i.e. to improve the liver’s ability to eliminate. The digestive system will also need clean-up. Thus detoxification would also be useful in addition.
With the patient in this kind of situation the first priority will be to improve detoxification and elimination and only then move on to antifungals. This will likely mean attention to enhancing liver activity, kidney activity and helping the lymph system.
Also this patient will have a longer road to recovery to go than the lady above. Being too aggressive too soon with antifungals initially may make this patient even more sick.
So one has to try to get some sort of decent interim improvement This is where anti-inflammatory/anti-infective treatments like ozone can really be useful and also intravenous vitamin and mineral infusions can help to get decent interim improvement for the patient while the long-term issues also are being worked on. This can be fantastic for giving a patient a good start back towards wellness. If it works well, the improvement can be very dramatic.
Then in the fullness of time it will also be necessary to use antifungals, reduced carbohydrate intake in the diet et cetera. One is hoping, also, that this gentleman’s prostatic symptoms also are likely because of fungus and may well disappear following treatment
The hope is that by the virtue of treating this person comprehensively, one could eliminate the fibromyalgia aches and pains /symptoms but also bring back energy for family, work and social life.
Get the patient sleeping well again, get the sinuses pretty well 100% under control , and treat the chemical sensitivity so that this person had a clear head, a well-functioning digestive system and a body that enabled him to do both his job and enjoy his family life, get his libido back and generally get on with things.
Despite the fact that in medicine we may classify fibromyalgia as one entity it really is just a symptom and the underlying causes differ very significantly from patient to patient. There is absolutely no one singular cause of fibromyalgia.